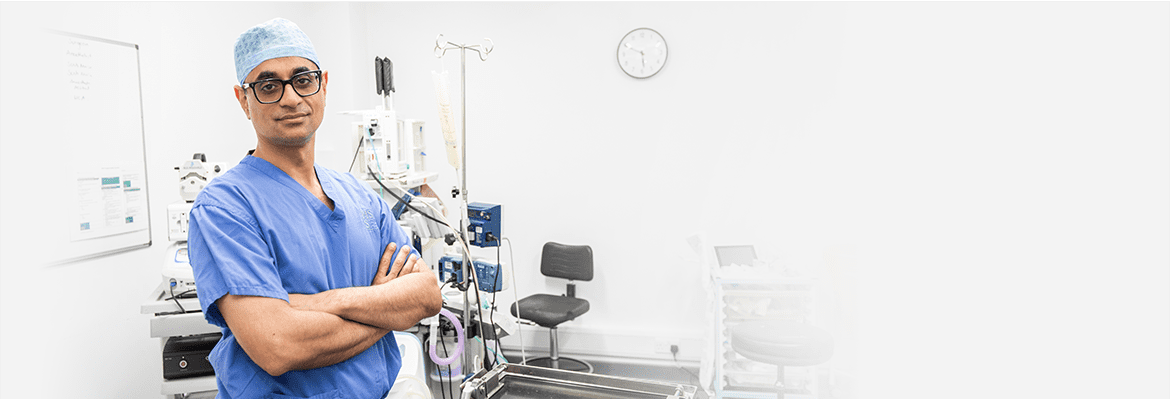
Mr. Sarvpreet Singh Consultant Orthopaedic Surgeon MBBS, MS (Orth), MRCS, Diploma in Sport & Exercise Medicine (Edin.), FRCS (Tr & Orth), MSc (University of Brighton).
Special Interests
- Knee Replacements including Revision Arthroplasty of the Knee
- ACL Reconstructions
- Meniscal Repair and Meniscectomy
- Hip Replacements
- Patello-Femoral joint surgery including Patello-Femoral Ligament Reconstructions
- Unicondylar (Half) Knee Replacements
- Knee Osteotomies
- N-Stride & Platelet Rich Plasma (PRP) injections
Mr. Sarvpreet SinghConsultant Orthopaedic Surgeon
MBBS, MS (Orth), MRCS, Diploma in Sport & Exercise Medicine (Edinburgh), FRCS (Tr & Orth), MSc (Brighton).
Mr. Sarvpreet Singh is a fellowship trained consultant orthopaedic surgeon with a special interest in knee and hip surgery that includes joint replacements and sports injuries.
He completed his specialist registrar training in orthopaedics on the London and South East Thames Rotation, this included working at Guy’s & St. Thomas’ Hospital in London along with other prominent hospitals on the south-east coast of England. This was followed by an internationally renowned fellowship at Exeter, in Devon. There he undertook training in all aspects of knee surgery that included knee replacement, osteotomies, and soft tissue surgery of the knee.
He furthered his training at the Frimley Park Hospital, in Surrey as a Fellow, undertaking more complex knee work and hip surgery.
After completing his Fellowships, he was appointed as a Consultant Trauma and Orthopaedic Surgeon for the North West Anglia NHS Foundation Trust in 2018, and currently works at Hinchingbrooke Hospital site. He was appointed as the Associate Medical Director of Patient Safety at the Trust in April 2020; and is also a member of the Thrombosis Committee of the Trust working on evaluating and formulating Trust Guidelines for VTE prevention.
Mr. Singh has completed a Master’s degree in Orthopaedics and a Diploma in Sports & Exercise Medicine. He has published in multiple peer-reviewed journals and has presented scientific papers both nationally and internationally. He sits as the orthopaedic representative on the Trust Research & Development Committee.
He is passionate about medical education and is the Undergraduate Lead for orthopaedic teaching at Hinchingbrooke Hospital for medical students from the School of Clinical Medicine, Cambridge. He is also actively involved in training overseas registrars on the Royal College of Surgeons exchange programme at Hinchingbrooke Hospital. He is a Senior Clinical Tutor at the University of Cambridge and a Fellow of the Academy of Medical Educators, UK.
He is recognised as a provider by all major healthcare insurers. He aims to provide a personalised service to his patients, and, works closely with a dedicated group of allied health-care professionals to deliver the best possible patient outcomes.
Outside of medicine, he enjoys cricket, tennis, golf, horse riding and wine.
Mr. Singh has private consulting chambers in Cambridge for a face-to-face consultation. Remote consultations on phone or video can also be arranged if needed.
NHS Service
Mr. Singh Consultant Orthopaedic Surgeon at Hinchingbrooke Hospital, part of North West Anglia NHS Foundation Trust.
Professional Positions
- Consultant Orthopaedic Surgeon, Hinchingbrooke Hospital, Cambridgeshire, UK.
- Champion of Flexible Working, Hinchingbrooke Hospital, Cambridgeshire, UK.
- Associate Medical Director for Patient Safety, North West Anglia NHS Foundation Trust.
- Member, Thrombosis Committee, North West Anglia NHS Foundation Trust.
- Orthopaedic Representative, Trust R&D Committee, North West Anglia NHS Foundation Trust.
- Senior Clinical Tutor, University of Cambridge, UK.
- Reviewer for Hodder Arnold Health Services Publishers, World Journal of Paediatrics and Royal Society of Medicine.
Research Interests
- ACL surgery and rehabilitation
- Patient satisfaction after knee replacement
- Dual mobility hip replacement
- Patellofemoral (knee cap) instability
- Orthobiologics
- Patient safety
Teaching Commitments
- University of Cambridge, UK– Senior Clinical Tutor and Undergraduate Lead for Orthopaedics at Hinchingbrooke Hospital, Cambridgeshire, UK.
- Academy of Medical Educators, UK– Fellow
- GKT Medical School, London– OSCE Examiner
- St. George’s Medical School, London– Problem/Case Based Tutor
- World Health Organisation- Global Initiative for Emergency and Essential Surgical Care (GIEESC) member - to help teach Orthopaedics & help the local authorities in setting up curriculum and protocols for emergency services
Committees
- Chair, Patient Safety Committee of the North West Anglia NHS Foundation Trust.
- Member, Thrombosis Committee at Hinchingbrooke Hospital, Cambridgeshire, UK.
- Orthopaedic Representative on the R & D Steering Committee of the North West Anglia NHS Foundation Trust.
- Editorial Board of Indian Journal of Orthopaedics (Ex-member).
Additional Languages Spoken
- Hindi - Native or bilingual
- Punjabi - Native or bilingual
- Gujarati - Native or bilingual
- Urdu - Native or bilingual
Personal Interests
Cricket, Tennis, Golf, Horse riding and Wine
Qualifications
- MSc, University of Brighton 2017
- FRCS (Tr & Orth), Royal College of Surgeons, UK & Northern Ireland 2014
- Diploma in Sport and Exercise Medicine, Royal College of Surgeons of Edinburgh 2008
- MRCS, Royal College of Surgeons of Edinburgh 2005
- MS (Orth), MS University 2000
- MBBS, MS University 1998
Professional Registration
- General Medical Council, 6026651
- Medical Council, Ireland, 427460
Specialist Fellowships
- Aug ‘17 – May ‘18; Fellow, Frimley Park Hospital, Frimley
- Aug ‘16 – Aug ‘17; Fellow, Royal Devon & Exeter Hospital, Exeter
Specialist Training – London & South East Thames Rotation
- Oct ‘14 – July ‘16; Eastbourne & Conquest Hospital, Hastings
- Oct ‘13 – Oct ‘14; William Harvey Hospital, Ashford
- Oct ‘12 – Oct ‘13; Guy’s & St. Thomas’ Hospital, London
- Oct ‘11 – Oct ‘12; Eastbourne DGH, Eastbourne
- Oct ‘10 – Oct ‘11; Royal Sussex County Hospital, Brighton
- Oct ‘09 – Oct ‘10; QEQM Hospital, Margate
Affiliations / Memberships
- British Orthopaedic Association
- British Association for Surgery of the Knee.
- European Society of Sports Traumatology, Knee Surgery, and Arthroscopy.
- British Patellofemoral Society.
- Academy of Medical Educators.
- British Medical Association
- Medical Protection Society
Publications
- Biomechanical testing of fixed and adjustable femoral cortical suspension devices for ACL reconstruction under high loads and extended cyclic loading. Singh S, Ramos-Pascual S, Czerbak, Malik M, Schranz PJ, Miles AW, Mandalia. Journal of Experimental Orthopaedics (2020); 7, Article number: 27.
- Adjustable loop femoral cortical suspension devices for anterior cruciate ligament reconstruction: A systematic review. Singh S, Shaunak S, Shaw SCK, Anderson JL, Mandalia V. Indian Journal of Orthopaedics, (2020); 54: Pages 426-43.
- Does laminar airflow make a difference to the infection rates for lower limb arthroplasty: A study using the England & Wales NJR and local SSI data for two hospitals with and without laminar airflow. Singh S, Reddy S, Shrivastava R. European J Orthop Surg Traumatol, (2017); 27: Pages 261-5.
- Complications of surgical management of fracture neck of femur. Singh S, Charles L, Changulani M. Orthopaedics and Trauma Journal, (2016); Vol 30, Issue 2: Pages 137-44.
- Challenges in reporting Surgical Site Infections (SSI) to the National Surgical Site Surveillance and suggestions for improvement. Singh S, Davies J, Sabou S, Shrivastava R, Reddy S. Ann R Coll Surg Engl, (2015), 97: Pages 460-5.
- Acute double flexor tendon ruptures following injection of Xiapex for Dupuytren’s contracture. Povlsen B, Singh S. BMJ Case Report, (2014): DOI: 10.1136/bcr-2013-203338.
- Initial management of open tibial fractures in DGH does not co-relate with increased failure rates – Letter to Editor. Lo S, Singh S, Soldin M. J Plast Reconstr Aesthetic Surgery, (2012); Vol 65, Issue 3: Page 401.
- Adherence to national guidelines on the management of open tibial fractures. Singh S, Lo S, Soldin M. Jour. of Evaluation of Clin. Practice, (2009); 15(6): Pages 1097-100.
- Arthroscopic powered instruments: a review of shavers and burrs. Singh S, Tavakkolizadeh A, Arya A, Compson J. Orthopaedics and Trauma Journal, (2009); 23(5): Pages 357-61.
- Cast and Padding Indices used for clinical decision making in forearm fractures in children. Singh S, Bhatia M, Housden P. Acta Orthopaedica Scandinavia, (2008); 79(3): Pages 386-89.
- VAC it! – Some technical tips on application of VAC dressing. Singh S, Mackey S, Soldin M. Ann R Coll Surg Engl, (2008), 90(2); Pages 161-2.
- Fifteen minute interview with Prof. Peter McCrorie, Head of Medical Education, St. George’s Medical School. Singh S. BMJ Careers, (2007); Page 203.
- Femoral stem displacement as a complication of reduction of a dislocated total hip arthroplasty. Rai P, Shrivastava R, Reddy GK, Singh S. European J Orthop Surg Traumatol, (2007); 17: Pages 207-9.
- Complications of pre-op India ink tattooing in colonic lesions. Singh S, Arif A, Fox C, Basnyat P. Digestive Surgery, (2006); 23 (5-6): Page 303.
- Periprosthetic fractures around resurfacing hip. Sinha S, Murthy A, Wijeratne M, Singh S, Housden PL. JBJS,(2006); Volume B88, B 2006: Orthopaedic Proceedings.
- Infusion of routinely stored blood may limit reperfusion injury to acutely ischaemic myocardium. Bagla N, Singh S, Mangal R. Medical Hypothesis, (2005); Vol 64, Issue 3: Pages 455-57.
Podium Presentations
- The biomechanical comparison of fixed v/s adjustable loops for ACL femoral suspension under high loads with extended cycles. Singh S, Ramos S, Czerbak, K, Miles T, Schranz P, Mandalia V. BASK Annual Spring Meeting in Stockport (2017): Short oral presentation session.
- Are our A&E patients requiring temporary immobilisation being assessed and prescribed VTE prophylaxis if appropriate? Singh S, Cheema T, Ganly K, Reed P, Armitage A. DOACON in Delhi, India (2015): Morning Session: Free papers.
- Soft tissue management of open distal third tibial fractures: free versus local flap cover. Singh S, Lo S, Soldin. BOA Annual Congress in Manchester (2007): Session 39: Free Papers Limb Reconstruction.
- Delays in flap coverage of open tibial fractures.Singh S, Lo S, Soldin M at Plastic Surgery Updates in French Alps (2007): Won Nagor Prize for Best Presentation.
- Enders Nail Versus Interlocking Nail for open tibial fractures. Singh S, Karthik V, Patel M, Daveshwar R. BOSA Annual Congress in Wrightington (2006): Afternoon Session.
- Can we predict the redisplacement of forearm and wrist fractures in children? Bhatia M, Singh S, Housden PL. BOA Annual Congress in Birmingham (2005); Session 32: Free Papers Trauma III.
- Periprosthetic fractures around resurfacing hip replacements. Sinha S, Murthy A, Wijeratne M, Singh S, Housden PL. EFFORT Congress in Lisbon (2005); Session 479: Hip 9.
Poster Presentations
- Is there a benefit to arthroscopy for patients destined for knee replacement? Flood C, Singh S, Shrivastava R. Association of Surgeons in Training (ASiT) Conference (2015), Glasgow.
- Informed Consent Study – Asking the patients if they were informed about the treatment options before consenting for surgery. Singh S, Mughal A, Yanni O. NHS Leadership Conference (2014), Queen Square, London
- Delays in the treatment of open tibial fractures: Where can we improve? Singh S, Lo S, Soldin M. British Trauma Society Annual Clinical Meeting (2007), Nottingham.
- Femoral stem displacement as a complication of reduction of a dislocated total hip replacement. Rai P, Singh S, Kumar, Shrivastava R. South East Thames Circuit Meeting (2005), Canterbury, Kent (2005).
- Canterbury Index for predicting redisplacement in paediatric forearm and wrist fractures. Bhatia M, Singh S, Housden PL. Fred Heatley Competition (2005), St. George’s Hospital, London (2005).
Audits
- NICE Guidelines on VTE Assessment in Orthopedic Patients Audit – Closing the loop on compliance with NICE guidelines on VTE Assessment timing for planned procedures (2019 & 2020). Getachew F, Singh S. Presented at the Clinical Governance meeting at Hinchingbrooke Hospital, Huntingdon.
- GMC Duties of a Good Doctor Audit – Personal audit of meeting GMC guidelines for working in partnership with patients (2016). Singh S. Discussed with my then Educational Supervisor for personal development.
- BOAST Fracture Clinic Audit – Compliance with the guidelines issued by BOAST for fracture clinic patients (2015). Wahed K, Singh S, Shrivastava R. Presented at the Trauma & Orthopaedics Audit meeting at William Harvey Hospital, Ashford.
- Acute Kidney Injury Audit – Causation of AKI in patients receiving pre-op teicoplanin and gentamycin for elective THR and TKR 92015). Wahed K, Cheema K, Singh S, Shrivastava R. Presented at the Trauma & Orthopaedics Audit meeting in William Harvey Hospital, Ashford.
- Ottawa Ankle Rules Audit – Compliance of these rules while ordering ankle radiographs in A&E Department of a DGH (2014). Ganly K, Singh S, Cheema T, Armitage A. Presented at the regional junior trainees conference for KSS Deanery in Eastbourne.
- Dr. Foster’s Data Audit – Accuracy of the surgeon specific data published on the website (2013). Singh S, Qureshi A, Housden P. Presented at the Trauma & Orthopaedics Audit meeting in William Harvey Hospital, Ashford.
- Pre-op Investigations audit - Closing the loop on excessive investigations ordered for elective orthopaedic surgery (2013). Altaf F, Singh S, Shah Z, Corbett S. Presented at the Trauma & Orthopaedics Audit meeting in Guy’s Hospital, London.
- Op Note Audit – Closing the loop on the quality and legibility of information on operative note (2012). Alwan S, Singh S, McNally S. Presented in the Trust Audit Meeting in, Eastbourne.
- VTE Audit – Closing the loop on VTE prophylaxis on an Orthopaedic rehab ward (2011). Singh S, Buddhdev S, Parnell E. Presented at the Clinical Governance meeting in RSC Hospital, Brighton.
- NOF Fast Track Audit – A prospective audit to identify delays in fast tracking uncomplicated fractures neck of femur to ward (2010). Singh S, Sindali K, Souied H, Smith A. Presented at the Trust wide Trauma & Orthopaedics Audit meeting in QEQM Hospital, Margate.
- Infection Audit – Retrospective audit on infection rates in THR/TKR at King’s College Hosp Aug 2005 – Jul 2006. (2007). Singh S, Stevenson J, Dodd L, Izadi E, Li P. Presented at the Trauma & Orthopaedics Audit Meeting in King’s College Hospital, London.
- Open Tibial Fracture Audit – Retrospective audit of 87 patients looking at flap cover time according to BOA-BAPS guidelines (2006). Singh S, Lo Steve, Odell E-K, Soldin M. Presented at the Plastic Surgery Clinical Governance Meeting in St. George’s Hospital, London.
- Consent Audit – Retrospective audit of sample of 212 patients incorporating relevant criteria from CNST & Trust consent (2005). Peppler F, Singh S et al. Presented at the Clinical Governance Committee at Kingston Hospital, Surrey.
- Belly Button Audit – Prospective audit about the junior doctor’s dressing in Poole Hospital (2004). Singh S, Massey L, Batcock TM. Presented at the Elderly Care Department at Poole Hospital, Dorset.
- Fracture Clinic Audit – Prospective audit on consultation time in fracture clinic (2003). Singh S, Blakeway C. Presented at the Orthopaedic Directorate Meeting at Poole Hospital, Dorset.